Total Knee Replacement
This procedure is most commonly used to treat severe osteoarthritis (OA) but can be used for other types of arthritis. Over 90,000 operations of this type are performed each year in the UK.
What is knee osteoarthritis (OA)?
As the surface cartilage becomes damaged, it thins and breaks. The damaged surfaces no longer cushion the knee and extra load goes on the bone surfaces. The damaged surface also provokes inflammation of the lining of the knee (synovitis), which adds to the pain, thickness of the tissues and extra fluid on the knee. The bone reacts by forming spurs (osteophytes) around the joint that contribute to the size and deformity of the knee and to stiffness. Once the surface is lost, it is frequently called ‘bone-on-bone’ arthritis.
Who gets knee osteoarthritis?
While it can run in families, many people are at increased risk of knee OA as a result of: obesity, increased age, previous knee injury, heavy manual jobs, increased activity levels, occupations that involve kneeling or squatting, and sports that involve high loading and twisting. Women are also more prone to OA than men.
When should you consider Total Knee Replacement (TKR)?
The decision whether to have a TKR should be taken by you but with advice and input from your knee surgeon and your family. It should be considered when other methods of managing your severe knee arthritis no longer give acceptable pain relief and function.
Usually patients will have tried: lifestyle modifications, weight loss, exercise, knee supports, cushioned insoles, sticks, liniments, hot or cold packs, pain killers, anti-inflammatory drugs, glucosamine, cod liver oil, and injections. Many with knee OA also feel it affects their mental wellbeing, their independence and their energy levels.
You are likely to benefit from TKR if you have:
- Severe knee pain that limits mobility and function
- Knee pain at rest or that disturbs your sleep
- Knee pain accompanied by progressive stiffness and deformity of the knee
Most patients who undergo total knee replacement are aged 55 to 80 but every patient’s symptoms, demands, expectations and risks are different and there is no specific upper or lower age limit for TKR. You will be assessed individually.
The operation
The procedure generally takes 1-2 hours and involves a cut over the front of the knee that is usually 10–20 cm long; this varies depending on the size of the leg and complexity of the surgery.
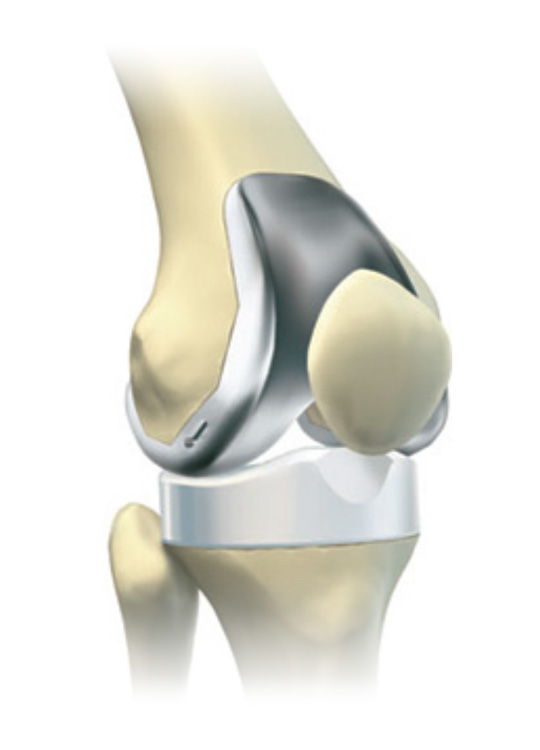
The surgeon then uses special instruments to remove the worn ends of the thigh bone and the top of the shin bone. Sometimes the surface of the kneecap is removed if it is badly damaged. The components of the knee replacement are then fixed to these surfaces, usually with bone cement. The femoral and tibial components are made out of metal (usually cobalt chrome for the femur and titanium for the tibia). A plastic block is then clipped into the tibial component and acts as a cushion between the metal surfaces. In patients with metal allergies, ceramic and plastic components can be used. In young or high demand patients, various modifications are available to try and reduce the risk of the TKR wearing out. Once the components are fixed in place and the ligaments balanced, the knee is closed with sutures or clips.
Knee Specialists surgeons have a long track record of being involved in the evaluation, development and research into numerous ways of improving techniques for and outcomes of knee replacement surgery. We strongly believe in bringing the best techniques and novel developments to our patients once there is a strong evidence base to support their use. New technologies are being developed all the time and your surgeon will be happy to discuss these with you.
Anaesthetic
Your anaesthetic consultant will discuss the types of anaesthetic that are best for you, but usually a general anaesthetic is combined with either an injection in the back, local anaesthetic blocks or local anaesthetic injections around the knee – these all help control any post-operative pain.
Recovery

You will be prescribed antibiotics (for 24 hours) and painkillers. The aim is to get you mobile as soon as possible to reduce the risk of stiffness and blood clots; as such you will have daily physiotherapy. To reduce the risk of blood clots, you will have compression stockings and foot pumps and will be given oral medication or injections to thin the blood. These are given when we are happy there is no risk of severe bleeding, and you may need to continue taking them after you go home. You are likely to be in hospital 3-5 days following the surgery. You will usually go home with sticks or crutches which you may need to use for a few weeks. The knee will still be swollen and warm and you may need to continue with elevation, ice and painkillers/anti-inflammatories for up to six weeks. Most people can consider driving at six weeks after a successful TKR and perhaps even a bit sooner if it was the left knee that was operated on or if you drive an automatic. You must feel you can safely do an emergency stop and control the car before you return to driving. It will take about three months before you feel you are really starting to recover from the operation; your movement, strength and walking speed will then continue to improve for about a year after surgery.
What are the risks?
The complication rate following total knee replacement is low. However, when complications do occur, they can prolong or limit your full recovery.
- Deep infection is a serious complication but occurs in less than 2% of cases.
- Medical complications such as heart attack or stroke occur even less frequently. Chronic illnesses may increase the potential for complications.
- Blood clots in the leg veins are the most common complication of knee replacement surgery. About 1 in 10 patients get a symptomatic clot in the calf and about 1 in 100 get an embolism to the lungs. Death from embolism after TKR is about 1 in 3000.
- Death from all causes in the first three months after TKR is less than 1 in 200.
- 1–2 % of patients experience stiffness following TKR that needs treatment.
- Injury to the nerves or blood vessels around the knee is rare.
- You can wear out the plastic or loosen a TKR from the bone, but over 90% will last over 10–15 years.
- It is common to get some skin numbness over the outer side of the scar – this may not fully recover.
- If you fall heavily in future, you can fracture the bones around the knee and loosen your knee replacement.
- About 1 in 10 patients will have some complications or ongoing pain after their TKR.
Realistic expectations after TKR
More than 90% of individuals who undergo total knee replacement experience a dramatic reduction of knee pain and a significant improvement in the ability to perform the common activities of daily life. There is often an improvement in walking speed and the distance that a person can cover. Many, but not all patients, will manage some exercise such as: walking, cycling, swimming, doubles tennis, dancing and golf. More vigorous sport is unlikely to be possible as it can cause the TKR to wear out quicker. Kneeling ability may improve slightly but most people still find kneeling difficult after TKR. Many patients never fully forget they have had a knee replacement and experience some ongoing symptoms or limitations.
